A Twist for Surgical Robotics
Larry Maloney | November 10, 2016Since 2000, California-based Intuitive Surgical has dominated the world of robot-assisted surgery. Its da Vinci system has logged well over two million surgical procedures.
Now, however, a Massachusetts startup called Medrobotics has launched a system of its own that features a design that could make robots a much more common fixture in operating rooms.
Rather than been being limited to straight, “line-of-sight” procedures as in other surgical robots, the company’s Flex Robotic System enables surgeons, with full HD visualization, to guide the device through the twists and turns of the body’s pathways. Result: minimally invasive surgery can be performed on sites that were difficult or even impossible to reach before.
 (Click to enlarge.) All the key components of the Flex Robotic System can be set up for surgery in about 10 minutes, say surgeons. The disposable Flex Drive (blue component) attaches to the Flex Base and is inserted into the patient.“With this system, we can now reach areas, such as the top of the voice box, which were very hard to access,” says Eugene Myers, M.D., a head and neck surgeon and professor at the University of Pittsburgh Medical School. “For example, this can mean the difference between a person losing his voice or retaining it.”
(Click to enlarge.) All the key components of the Flex Robotic System can be set up for surgery in about 10 minutes, say surgeons. The disposable Flex Drive (blue component) attaches to the Flex Base and is inserted into the patient.“With this system, we can now reach areas, such as the top of the voice box, which were very hard to access,” says Eugene Myers, M.D., a head and neck surgeon and professor at the University of Pittsburgh Medical School. “For example, this can mean the difference between a person losing his voice or retaining it.”
So far, the Flex Robotic System has received both U.S. Food and Drug Administration approval and Europe’s CE mark for transoral procedures of the mouth and throat. In October 2016, the system also gained European clearance for colorectal surgeries, expanding the range of operations. Costing about $1 million--around half the price of the latest da Vinci model--the system offers a relatively small footprint and a reported 10-minute setup time in operating rooms.
The device is gaining recognition, including a Best of Show award in the 2016 Medical Design Excellence Awards, and a 2016 Red Herring Top 100 Award, which recognizes technologies most likely to change people’s lives. Meanwhile, the technology has attracted about $150 million in investment for Medrobotics.
“The global market for robotics and other tools for minimally invasive surgery is expected to double by 2020,” says James Jordan, chief investment officer for Pittsburgh Life Sciences Greenhouse, an early investor in Medrobotics. “But that type of increase is not likely to occur without flexible robotics technology.”
Roots at Carnegie Mellon
The Medrobotics story began at Carnegie Mellon University’s Robotics Institute, which has spawned robotics innovations ranging from devices to inspect power plants and explore space environments to autonomous tractors and self-driving cars. (Read Part 1 and Part 2 of our conversation with the Institute's legendary William “Red” Whittaker.)
 Professor Howie Choset of Carnegie Mellon University’s Robotic Institute developed the core motion system for flexible robotics.In the late 1990s, Robotics Institute engineering professor Howie Choset became fascinated with what has become known as “snake robots,” highly-articulated mechanisms with many degrees of freedom. These robotic snakes can thread their way through tightly packed areas in such applications as search and rescue missions and the manufacture of giant aircraft wings.
Professor Howie Choset of Carnegie Mellon University’s Robotic Institute developed the core motion system for flexible robotics.In the late 1990s, Robotics Institute engineering professor Howie Choset became fascinated with what has become known as “snake robots,” highly-articulated mechanisms with many degrees of freedom. These robotic snakes can thread their way through tightly packed areas in such applications as search and rescue missions and the manufacture of giant aircraft wings.
Along with fellow CMU engineering professor Alon Wolf and heart surgeon Marco Zenati, M.D., Choset developed the first prototype of a snake robot for minimally invasive surgery.
Together, the three men founded Medrobotics in 2005. They initially targeted the device for heart surgery, and it was used successfully in a limited investigational trial on three patients in Europe in 2010. It became apparent, however, that the high cost of developing a commercial device for cardiac applications, as well as the regulatory hurdles, dictated moving to other surgical procedures for faster commercial launch.
Noting that commercializing a surgical device is “not something that a robotics professor can accomplish with grants to the university,” Choset knew it was time to hand off his invention to Medrobotics. The company not only had to raise an enormous amount of capital for development and manufacturing infrastructure, but its engineers had to refine Choset’s design, both to pass muster with regulators and to meet the clinical demands of surgeons.
“The genius of Professor Choset’s design was his revolutionary motion system, specifically the relationship of the inner and outer mechanisms of the robot that allows the articulation to occur, just like a snake,” says Samuel Straface, a Ph.D. and former scientist who serves as president and CEO of Medrobotics. “Our engineers had to transfer that know-how into a viable product for clinicians.”
Follow the Leader
The Flex Robotics System that received FDA clearance in July 2015 combines the benefits of a laparoscope – a rigid, straight-viewing device used in minimally-invasive surgery -- with an endoscope, a flexible instrument for visual diagnosis.
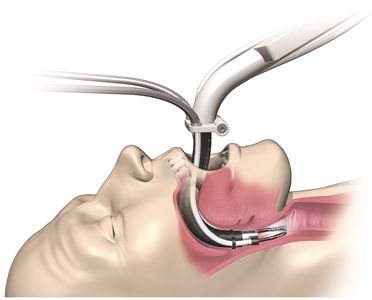 Illustration shows the key advantage of the Flex Robotic System: the ability to navigate through the body’s twists and turns to hard-to-reach surgical sites.Much of the device’s intellectual property revolves around the disposable Flex Drive, which snaps into a reusable base that contains system motors and controls. For transoral applications, the portion of the 1.5-lb drive inserted into the patient and containing the camera measures about 17 cm long, with a diameter that ranges from 17.5 mm to a maximum of 28 mm at the “distal end” where the surgery takes place.
Illustration shows the key advantage of the Flex Robotic System: the ability to navigate through the body’s twists and turns to hard-to-reach surgical sites.Much of the device’s intellectual property revolves around the disposable Flex Drive, which snaps into a reusable base that contains system motors and controls. For transoral applications, the portion of the 1.5-lb drive inserted into the patient and containing the camera measures about 17 cm long, with a diameter that ranges from 17.5 mm to a maximum of 28 mm at the “distal end” where the surgery takes place.
The drive contains an external cable for electrical connections to the distally mounted, detachable camera and LEDs, plus an internal lumen that serves as a channel for tubing that carries fluid to a lens washer for the camera. The Flex Drive also contains accessory channels on either side of the camera to accommodate miniature instruments that the surgeon inserts during an operation.
At the heart of the Flex Drive’s technology is its motion system, which features a series of articulated segments or links. The design includes both inner and outer articulated segments, made of medical-grade polymer and arranged in a concentric mechanical assembly.
The control scheme causes each of these two assemblies to become semi-rigid or flexible by adjusting the tension on cables running through the segments. The outer assembly can also be articulated by varying the tension on its cables when part of it moves beyond the distal end of the inner assembly.
Using this ‘‘follow-the-leader’’ strategy and alternating flexible and rigid states, the drive moves to the surgical site under the direct control of the surgeon (watch this video). Once positioned, the device can become rigid, forming a stable surgical platform.
 As R&D chief, engineer Russell Singleton heads the multidisciplinary team that has turned the “snake robot” concept into an FDA-approved medical device. A key distinguishing feature of this flexible robot is that it offers multiple degrees of freedom distributed across its length. When compared to the typical human arm’s 7 degrees of freedom, the device’s more than 30 degrees of freedom may enhance the physician’s ability to access, visualize, and perform surgeries.
As R&D chief, engineer Russell Singleton heads the multidisciplinary team that has turned the “snake robot” concept into an FDA-approved medical device. A key distinguishing feature of this flexible robot is that it offers multiple degrees of freedom distributed across its length. When compared to the typical human arm’s 7 degrees of freedom, the device’s more than 30 degrees of freedom may enhance the physician’s ability to access, visualize, and perform surgeries.
And unlike other robotic systems, where the surgeon sits at a console several feet away from the operating table, the physician sits or stands next to the patient and uses a joy-stick-like controller on an adjacent console to move the inserted scope to the surgical site. A touchscreen monitor shows system operation, and a video display provides real-time, 3D visualization of the surgery.
Once the robot reaches the surgical site, the surgeon manipulates two other controllers, one in each hand, that control tiny instruments inserted through the Flex Drive’s two accessory channels. For example, the instrument controlled by the left hand might grasp a piece of tissue, while the instrument controlled by the right excises tissue for a biopsy. What’s more, the surgeon gets haptic feedback throughout the procedure.
Meeting the Engineering Challenge
Bringing the Flex Robotic System to its current state of the art has required a strategy of agile engineering, notes R&D director Russell Singleton, a Ph.D. electrical engineer whose career has included many years with startups. “The approach is to get the design out as fast as you can, then do more iterations as you go along, based on the needs of the application.”
The team also features a blend of engineering disciplines. “There is no mechanical engineering department, or electrical engineering department,” notes Singleton. “We are organized by project or program, and we encourage the cross-fertilization of ideas.”
Singleton says he prefers to buy as many components as he can off the shelf. However, the unique demands of this flexible system have dictated several homegrown designs. Since the second half of 2014, when the Flex Robotic System debuted in Europe for transoral applications, company engineers have made significant changes in the design of key components.
The “chip-on-tip” camera, which snaps onto the distal end of the Flex Drive, has evolved from a disposable, 800 x 800 pixel 2-D version to the current dual 1920 x 1080-pixel, high-definition 3D model that can be detached, sterilized and reused.
 The distal end of the Flex Drive includes the camera, LEDs, and accessory channels through which the surgeon inserts custom-designed instruments.With a goal of creating a much more mobile and nimble platform, engineers have also reduced the size and weight of the Flex Drive to one tenth of what it was in 2014. In addition, based on the input of surgeons who work closely with the company, engineers have created a family of miniature surgical instruments that are disposable and measure just 3.5 mm in outer diameter. Some specialized instruments for operating on the voice box have diameters as small as 1.5 mm. Moreover, engineers have had to design these instruments to be flexible, since they too must navigate through channels that bend and twist to fit the body’s anatomy.
The distal end of the Flex Drive includes the camera, LEDs, and accessory channels through which the surgeon inserts custom-designed instruments.With a goal of creating a much more mobile and nimble platform, engineers have also reduced the size and weight of the Flex Drive to one tenth of what it was in 2014. In addition, based on the input of surgeons who work closely with the company, engineers have created a family of miniature surgical instruments that are disposable and measure just 3.5 mm in outer diameter. Some specialized instruments for operating on the voice box have diameters as small as 1.5 mm. Moreover, engineers have had to design these instruments to be flexible, since they too must navigate through channels that bend and twist to fit the body’s anatomy.
“Medrobotics’ engineers are not only dedicated and talented, but they are used to fast turnaround,” notes Marshall Strome, M.D., a professor and chairman emeritus of the Cleveland Clinic Head and Neck Institute. “I recall cases where I asked engineers in the morning to modify an instrument, and they had a new design to show me by the end of the day.”
The engineers also must tackle the tough task of developing motion control and path planning algorithms, a particularly challenging job in snake robot systems with their multiple degrees of freedom. Singleton cites MATLAB as a useful software package to model and simulate motion and path planning. Among other key tools: SOLIDWORKS for 3D CAD modeling of components and Altium for printed circuit board design.
Ramping Up for Production
On the manufacturing side, the Flex Robotics System must run a gauntlet of tests needed for regulatory approval. The battery of tests described in the company’s 510 (k) premarket submission to the FDA in 2015 include: electrical safety testing, biocompatibility, sterilization and packaging, animal studies, and human factors testing, among other things. As production ramps up, clean rooms, both at Raynham and offsite, will be used to assemble the camera, as well as disposable components, such as the Flex Drive and surgical instruments.
Michael Gallagher, the Medrobotics’ vice president of Operations, says the Flex Robotic System requires about 3,000 components, which presents challenges in materials and resource planning. Continuing design changes trigger additional adjustments in manufacturing.
For example, the move to 3-D vision requires changes in the Flex Base, such as replacing multiple circuit boards and machining of the frame. Meanwhile, field upgrades to systems installed in hospitals have to be managed. “It’s a very fast-paced environment, like being strapped to a rocket, and you have to be agile,” says Gallagher.
 Medrobotics CEO Samuel Straface says that rapid growth in surgical robotics will depend on the adoption of flexible systems.To manage such tasks, Gallagher cites QAD software as an important tool in materials and resource planning. In 2017, the company plans to introduce Omnify product lifecycle management software, a package that includes quality assurance features. On the test side, Gallagher points to software packages like LabVIEW TestStand and Euresys, both used in important tests of the Flex Drive’s camera lens.
Medrobotics CEO Samuel Straface says that rapid growth in surgical robotics will depend on the adoption of flexible systems.To manage such tasks, Gallagher cites QAD software as an important tool in materials and resource planning. In 2017, the company plans to introduce Omnify product lifecycle management software, a package that includes quality assurance features. On the test side, Gallagher points to software packages like LabVIEW TestStand and Euresys, both used in important tests of the Flex Drive’s camera lens.
Throughout the system’s development, Medrobotics has embedded manufacturing engineers and supply chain managers alongside design engineers on project teams, says Gallagher, both to optimize components for production and test, as well as to ensure better resource planning. For example, engineers configured complex boards on camera assemblies for more efficient testing on bed-of-nails fixtures. To reduce costs and simplify production, the engineering team completely redesigned the Flex Drive, replacing custom-machined components with injection molded parts.
Growth Spurt
As Medrobotics positions its system for new surgical applications, engineers will need to make further design and manufacturing changes, including the size and shape of the Flex Drive, new types of surgical instruments, the configuration of special retractors and fixtures through which the drive enters a patient, and motion control and path planning.
Still, the company is confident that it will play a major role in the growth of surgical robots in the years ahead. Nearly every day, surgeons can be found at the Raynham facility, where four complete systems have been set up to acquaint medical personnel with the technology. Surgeons, such as Dr. Umamaheswar Duvvuri of the University of Pittsburgh School of Medicine and Dr. David Goldenberg of the Penn State College of Medicine, are demonstrating the system to interested surgeons in surgical settings.
In addition, surgeons in Europe are helping to prove the technology’s viability. In July 2016, Medrobotics released the results of clinical trials involving 80 patients with throat lesions at four hospitals in Germany and Belgium. Using the Flex Robotic System, surgeons accessed the target area in 94% of the cases. No device-related adverse events were reported.
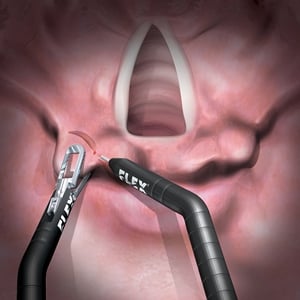 Illustration shows the system’s miniature instruments at a surgical site. The array of Medrobotics-designed instruments will expand with new surgical applications.Surgeons familiar with the system point to such benefits as being able to see behind anatomical structures, such as organs, to detect hidden tumors. They add that flexible robotics also helps them perform more precise surgery, which can mean reduced need for chemo and radiation therapies in cancer patients.
Illustration shows the system’s miniature instruments at a surgical site. The array of Medrobotics-designed instruments will expand with new surgical applications.Surgeons familiar with the system point to such benefits as being able to see behind anatomical structures, such as organs, to detect hidden tumors. They add that flexible robotics also helps them perform more precise surgery, which can mean reduced need for chemo and radiation therapies in cancer patients.
Encouraged by the response from the medical community, CEO Straface expects to see several hundred hospitals worldwide using the Flex Robotic system within the next three years. Beyond transoral and colorectal applications, he sees the device being used in an expanding array of procedures, such as gynecological surgery. Eventually, he believes surgeons will choose flexible robotics for operations on the beating heart.
With an intellectual property portfolio that includes 200 patents issued or pending, Straface says his company has achieved “hard won” leadership in the field of flexible robotics for medical applications.
“Analysts are predicting a mammoth rise in the adoption of robots for surgery,” says Straface. But for that to happen, he says that a paradigm shift must occur so that surgeons “are no longer limited to line-of-sight robotic technology.”




